SARS-CoV-2 Vaccination and Myocarditis in a Nordic Cohort Study of 23 Million Residents
Key PointsQuestion Is SARS-CoV-2 messenger RNA (mRNA) vaccination associated with risk of myocarditis?
Findings In a cohort study of 23.1 million residents across 4 Nordic countries, risk of myocarditis after the first and second doses of SARS-CoV-2 mRNA vaccines was highest in young males aged 16 to 24 years after the second dose. For young males receiving 2 doses of the same vaccine, data were compatible with between 4 and 7 excess events in 28 days per 100 000 vaccinees after second-dose BNT162b2, and between 9 and 28 per 100 000 vaccinees after second-dose mRNA-1273.
Meaning The risk of myocarditis in this large cohort study was highest in young males after the second SARS-CoV-2 vaccine dose, and this risk should be balanced against the benefits of protecting against severe COVID-19 disease.
Abstract
Importance Reports of myocarditis after SARS-CoV-2 messenger RNA (mRNA) vaccination have emerged.
Objective To evaluate the risks of myocarditis and pericarditis following SARS-CoV-2 vaccination by vaccine product, vaccination dose number, sex, and age.
Design, Setting, and Participants Four cohort studies were conducted according to a common protocol, and the results were combined using meta-analysis. Participants were 23 122 522 residents aged 12 years or older. They were followed up from December 27, 2020, until incident myocarditis or pericarditis, censoring, or study end (October 5, 2021). Data on SARS-CoV-2 vaccinations, hospital diagnoses of myocarditis or pericarditis, and covariates for the participants were obtained from linked nationwide health registers in Denmark, Finland, Norway, and Sweden.
Exposures The 28-day risk periods after administration date of the first and second doses of a SARS-CoV-2 vaccine, including BNT162b2, mRNA-1273, and AZD1222 or combinations thereof. A homologous schedule was defined as receiving the same vaccine type for doses 1 and 2.
Main Outcomes and Measures Incident outcome events were defined as the date of first inpatient hospital admission based on primary or secondary discharge diagnosis for myocarditis or pericarditis from December 27, 2020, onward. Secondary outcome was myocarditis or pericarditis combined from either inpatient or outpatient hospital care. Poisson regression yielded adjusted incidence rate ratios (IRRs) and excess rates with 95% CIs, comparing rates of myocarditis or pericarditis in the 28-day period following vaccination with rates among unvaccinated individuals.
Results Among 23 122 522 Nordic residents (81% vaccinated by study end; 50.2% female), 1077 incident myocarditis events and 1149 incident pericarditis events were identified. Within the 28-day period, for males and females 12 years or older combined who received a homologous schedule, the second dose was associated with higher risk of myocarditis, with adjusted IRRs of 1.75 (95% CI, 1.43-2.14) for BNT162b2 and 6.57 (95% CI, 4.64-9.28) for mRNA-1273. Among males 16 to 24 years of age, adjusted IRRs were 5.31 (95% CI, 3.68-7.68) for a second dose of BNT162b2 and 13.83 (95% CI, 8.08-23.68) for a second dose of mRNA-1273, and numbers of excess events were 5.55 (95% CI, 3.70-7.39) events per 100 000 vaccinees after the second dose of BNT162b2 and 18.39 (9.05-27.72) events per 100 000 vaccinees after the second dose of mRNA-1273. Estimates for pericarditis were similar.
Conclusions and Relevance Results of this large cohort study indicated that both first and second doses of mRNA vaccines were associated with increased risk of myocarditis and pericarditis. For individuals receiving 2 doses of the same vaccine, risk of myocarditis was highest among young males (aged 16-24 years) after the second dose. These findings are compatible with between 4 and 7 excess events in 28 days per 100 000 vaccinees after BNT162b2, and between 9 and 28 excess events per 100 000 vaccinees after mRNA-1273. This risk should be balanced against the benefits of protecting against severe COVID-19 disease.
Introduction
The European Medicines Agency and European Commission have, by October 2021, approved 4 vaccines against SARS-CoV-2: BNT162b2 (Pfizer-BioNTech), mRNA-1273 (Moderna), AZD1222 (AstraZeneca), and Ad26.COV2.S (Janssen). The Nordic countries have primarily used the 2 messenger RNA (mRNA) vaccines BNT162b2 and mRNA-1273. These vaccines have been shown to be efficient and safe, although cases of myocarditis or pericarditis during the first weeks after vaccination have been reported.1
Case reports, surveillance data, and other reports from the US, Israel, and Canada indicate an increased risk of myocarditis after vaccination with SARS-CoV-2 mRNA vaccines, higher after the second dose, especially in younger men.2–9 Data from Canada and France indicate more cases of myocarditis after mRNA-1273 than after BNT162b2, but this remains to be elucidated.10,11
In nationwide cohort studies in Denmark, Finland, Norway, and Sweden, we evaluated the risks of myocarditis and pericarditis following SARS-CoV-2 vaccination in a combined population of 23.1 million individuals. High-quality nationwide registers enabled us to evaluate the risk by vaccine product, vaccination dose number, sex, and age.
Methods
We conducted population-based cohort studies in 4 Nordic countries (Denmark, Finland, Norway, and Sweden) using linked data from nationwide health registers on SARS-CoV-2 vaccination, myocarditis and pericarditis diagnoses, and other covariates (eMethods in the Supplement). All Nordic residents are assigned a unique personal identifier at birth or immigration, enabling deterministic linkage between registers. These countries have universal and tax-financed health care systems, and reporting to national registers is mandatory, providing near-complete follow-up of all residents over time.12,13 Each cohort study was analyzed separately according to a common protocol, and the results were combined by meta-analyses. On the basis of current law in each of the countries, this register-based research was conducted according to the laws, regulations, and authority permits, and informed consent from individuals was not applicable (eMethods in the Supplement).14 The requirement for obtaining informed consent was waived because all data are publicly available. This study followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guideline.
Study Population
We included all persons who turned 12 years or older in 2021, were residents on January 1, 2017, and were alive and still residing within the country on December 27, 2020. We excluded 20 211 persons with any myocarditis or pericarditis in inpatient or outpatient hospital care from January 1, 2017, to December 26, 2020 (eMethods in the Supplement).
SARS-CoV-2 Vaccination
The Nordic countries implemented national vaccination campaigns against SARS-CoV-2 from December 27, 2020, providing free vaccinations to all residents. Phased distribution plans were implemented, prioritizing vaccination of individuals at highest risk of COVID-19 complications (ie, nursing home residents, health care workers, and older adults). Denmark, Finland, and Norway almost exclusively used mRNA vaccines after full or partial discontinuation of AZD1222 in March 2021 because of serious but rare events of thrombosis with thrombocytopenia.15,16 Sweden used AZD1222 for a majority of the population older than 64 years and mRNA vaccines in other age groups. The vaccine Ad26.COV2.S had very limited use. The Nordic countries vaccinated approximately 6 times more individuals with BNT162b2 than with mRNA-1273 because of higher availability of the former vaccine. We studied risk of myocarditis and pericarditis in 28-day risk periods after the administration date of the first and second dose with BNT162b2, mRNA-1273, and AZD1222 (Figure 1). A homologous schedule was defined as receiving the same vaccine type for doses 1 and 2.
Myocarditis and Pericarditis
We defined incident outcome events as the date of first hospital admission for myocarditis or pericarditis from December 27, 2020, onward. The primary outcome was a main or secondary diagnosis of myocarditis at discharge from inpatient hospital care. Secondary outcomes were a main or secondary diagnosis of pericarditis (inpatient hospital care) and a main or secondary diagnosis of either condition (myocarditis or pericarditis) combined from either inpatient or outpatient hospital care (eTable 1 in the Supplement).
Covariates
We used the following covariates for adjustment and stratification: sex, age, calendar period, health care worker status, nursing home resident, and 5 comorbidities (pulmonary disease, kidney disease, autoimmune disease, cardiovascular disease or diabetes, and cancer) defined by diagnoses before the start of follow-up (eTable 2 in the Supplement). We also adjusted for verified SARS-CoV-2 infection before December 27, 2020, whereas infection after this date was a censoring event. We defined having SARS-CoV-2 as the sample date of a positive reverse transcriptase–polymerase chain reaction or lateral flow test.
Statistical Analysis
We took advantage of the longitudinal information in our national cohorts to calculate exact unvaccinated and vaccinated person-time at risk for each individual (Figure 1). We started follow-up on December 27, 2020. Each individual was followed up until first outcome event of interest or a censoring event, defined as first occurrence of a positive test result for SARS-CoV-2 infection, receiving Ad26.COV2.S vaccine, receiving a third dose of any SARS-CoV-2 vaccine, emigration, death, or country-specific study end (latest October 5, 2021). Individuals contributed person-time as unvaccinated until the first vaccination. After each first or second dose, individuals contributed person-time in a main risk period of interest defined as day 0 up to and including day 28 (Figure 1). The resulting follow-up periods and numbers of myocarditis and pericarditis cases were aggregated for all individuals according to vaccination status (ie, unvaccinated, risk period after first dose, and risk period after second dose).
We used Poisson regression for the number of events to estimate incidence rate ratios (IRRs) with 95% CIs, comparing rates in the risk periods after vaccination with rates in unvaccinated periods. We took potential confounding factors into account by adjustment in 3 models. Model 1 included adjustment for sex and age group (12-15, 16-19, 20-24, 25-29, 30-39, 40-64, and ≥65 years). Model 2 included adjustment as in model 1 and for health care worker status, nursing home resident, and the aforementioned comorbidities. Model 3 included adjustment as in model 2 and for calendar periods (December through March, April through June, and July to the study end). We used model 2 in the main analyses, whereas models 1 and 3 were used for sensitivity analyses. We included subgroup results according to sex and age (12-15, 16-24, 25-39, and ≥40 years). Analyses were conducted in Denmark and Sweden with SAS, version 9.4 (SAS Institute Inc), in Finland with R, version 3.6.3 (R Foundation for Statistical Computing), and in Norway with Stata, version 16.0 (StataCorp LLC).
Meta-analyses
Meta-analyses of the IRR estimates were based on random-effects models implemented using the mixmeta package17 of R.18 We tested the homogeneity of country-specific estimates using the Cochran Q test,19 calculated the pooled incidence rates using the sum of events and person-years in the countries, and calculated the pooled excess rates using the pooled incidence rates and IRR estimates. For the CIs, we used the delta method, assuming independence of the incidence rates and IRR estimates.
Supplementary Analyses
In a complementary analysis, we studied incident myocarditis within 28 days following SARS-CoV-2 infection from August 1, 2020, to end of study. We also studied risk of myocarditis or pericarditis in a shorter 7-day risk period. Furthermore, among myocarditis cases, we estimated the proportion of patients discharged on day 4 or later and the proportion of cases in which the patient died within 28 days of the admission date, using the Kaplan-Meier estimator. Among myocarditis cases after vaccination, we calculated the median time from vaccination to outcome (hospital admission date).
Results
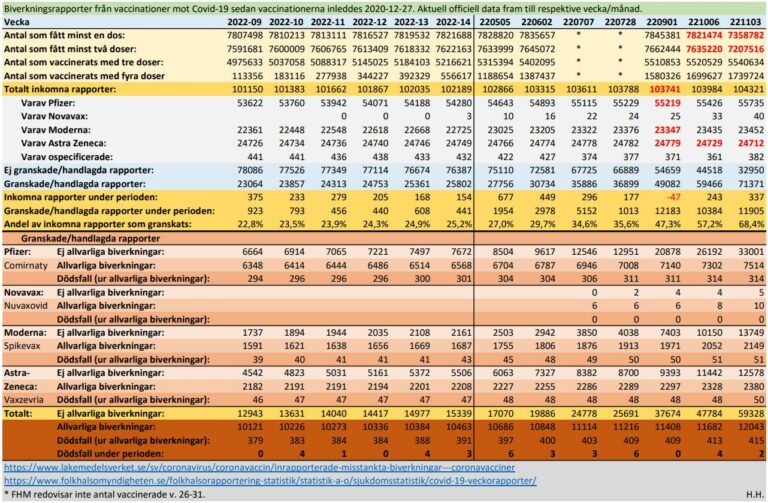
Across 4 Nordic countries, 23 122 522 residents (49.8% male and 50.2% female) were followed up from December 27, 2020, to October 5, 2021, at the latest. By study end, 17 129 982 residents (74%) had received 2 doses and 1 681 930 residents (7%) had received 1 dose of SARS-CoV-2 vaccines. By study end, 487 751 of 1 238 004 persons (39%) aged 12 to 15 years, 2 009 995 of 2 675 558 persons (75%) aged 16 to 24 years of age, 3 736 517 of 5 046 164 persons (74%) aged 25 to 39 years, and 12 579 805 of 14 162 796 persons (89%) aged 40 years or older had received at least 1 dose of a SARS-CoV-2 vaccine (Table 1; eTable 3 in the Supplement).
Myocarditis and Pericarditis During Follow-up
During the 28-day risk periods following vaccination and during unvaccinated periods (13 million person-years in total), we observed 1077 incident myocarditis cases and 1149 incident pericarditis cases. Incidence rates of myocarditis during the unvaccinated period were 9.7 per 100 000 person-years for males and 4.3 per 100 000 person-years for females (Table 2). Among individuals aged 16 to 24 years, incidence rates were 18.8 per 100 000 person-years for males and 4.4 per 100 000 person-years for females. Incidence rates of pericarditis increased with age (eTable 4 in the Supplement).
Vaccination and Myocarditis
During the 28-day risk period, we observed 105 myocarditis cases following administration of the first dose of BNT162b2 and 115 myocarditis cases following the second dose. We also observed 15 myocarditis cases following administration of the first dose of mRNA-1273 and 60 myocarditis cases following the second dose.
Adjusted IRRs comparing the 28-day risk periods following first and second doses compared with unvaccinated periods were 1.38 (95% CI, 1.12-1.69) for the first dose of BNT162b2 and 1.75 (95% CI, 1.43-2.14) for the second dose, and 1.16 (95% CI, 0.69-1.93) for the first dose of mRNA-1273 and 6.57 (95% CI, 4.64-9.28) for the second dose. Among males, after the first and second doses, adjusted IRRs were 1.40 (95% CI, 1.09-1.80) for the first dose of BNT162b2 and 2.04 (95% CI, 1.61-2.58) for the second dose, and 1.45 (95% CI, 0.84-2.52) for the first dose of mRNA-1273 and 8.55 (95% CI, 6.40-11.41) for the second dose. Among females, following the first and second doses, adjusted IRRs were 1.46 (95% CI, 1.01-2.11) for the first dose of BNT162b2 and 1.25 (95% CI, 0.77-2.05) for the second dose, and 1.45 (95% CI, 0.35-5.97) for the first dose of mRNA-1273 and 2.73 (95% CI, 1.27-5.87) for the second dose.
Among males 16 to 24 years of age, the adjusted IRRs for myocarditis were 5.31 (95% CI, 3.68-7.68) for a second dose of BNT162b2 and 13.83 (95% CI, 8.08-23.68) for a second dose of mRNA-1273. For females, the comparative adjusted IRRs were lower (Table 2, Figure 2, Figure 3; eFigure 1 in the Supplement).
We also estimated the excess numbers of myocarditis events per 100 000 vaccinees in the 28-day risk periods. Among all males, these numbers were 0.27 (95% CI, 0.09-0.46) events after the first dose of BNT162b2 and 0.67 (95% CI, 0.46-0.88) events after the second dose, and 0.33 (95% CI, −0.11 to 0.78) events after the first dose of mRNA-1273 and 4.97 (95% CI, 3.62-6.32) events after the second dose. Among all females, the excess numbers of events per 100 000 vaccinees in the 28-day risk periods were 0.15 (95% CI, 0.02-0.28) events after the first dose of BNT162b2 and 0.09 (95% CI, −0.09 to 0.26) events after the second dose, and 0.05 (95% CI, −0.13 to 0.23) events after the first dose of mRNA-1273 and 0.48 (95% CI, 0.07-0.89) events after the second dose (Table 2).
Among males 16 to 24 years of age, the excess number of myocarditis events per 100 000 vaccinees in the 28-day risk periods after the first dose of BNT162b2 was 1.55 (95% CI, 0.70-2.39) events and after the second dose was 5.55 (95% CI, 3.70-7.39) events, and it was 1.75 (95% CI, −0.20 to 3.71) events after the first dose of mRNA-1273 and 18.39 (95% CI, 9.05-27.72) events after the second dose (Table 2).
For a heterologous schedule (1 dose with BNT162b2 and the other dose with mRNA-1273), 38 myocarditis cases (34 males) occurred following the second dose, with an excess number of events in males of 10.34 (95% CI, 6.86-13.83) events. In males aged 16 to 24 years, 17 myocarditis cases occurred, with an excess number of events of 27.49 (95% CI, 14.41-40.56) events (Table 2).
Vaccination and Pericarditis
Pericarditis in males followed a pattern similar to myocarditis by vaccine product and age but with lower IRRs. Pericarditis was rare in females aged 12 to 39 years. Among males aged 16 to 24 years of age, the excess number of pericarditis events within the 28-day risk period was 7.39 per 100 000 vaccinees (95% CI, 1.46-13.32) events for the second dose of mRNA-1273 (eTables 4 and 5 in the Supplement).
Vaccination and Myocarditis or Pericarditis Combined
The IRRs of myocarditis or pericarditis combined among males aged 16 to 24 years were slightly higher than those of myocarditis (Table 3). In males aged 25 to 39 years, the IRRs were generally lower. Among females aged 16 to 24 years, the IRRs were similar to those for males but with fewer events. Among males aged 12 to 15 years, the crude IRR was based on very few events among the vaccinated population (eTable 6 in the Supplement).
SARS-CoV-2 Infection and Myocarditis
During the 28-day risk period after a positive SARS-CoV-2 test, there were 73 myocarditis cases. Excess events of myocarditis were 3.26 (95% CI, 1.90-4.61) events per 100 000 individuals with a positive test result among all males, and 1.37 (95% CI, −0.14 to 2.87) events per 100 000 individuals with a positive test result among males aged 16 to 24 years (eTable 7 in the Supplement).
Supplementary Analyses
The IRRs and excess rates were slightly attenuated when model 1 was complemented by other covariates (model 2) and further attenuated when calendar period was added (model 3) (eFigure 2 and eTable 5 in the Supplement). Among males aged 16 to 24 years, adjustment for calendar period (model 3) yielded unstable point estimates with wide CIs for the second dose of mRNA-1273. Heterogeneity of the analyses across countries was not statistically significant (eFigure 2 in the Supplement); thus, we present the results as pooled 4-country estimates of IRRs and excess rates.
Of the 213 myocarditis cases in the 28-day risk window after a second dose of SARS-CoV-2 mRNA vaccination, 135 events occurred within the first week, yielding higher IRRs in the 7-day risk period (Table 2; eTable 8 in the Supplement). Among males aged 16 to 24 years, the adjusted IRRs were 12.50 (8.24-18.96) for a second dose of BNT162b2 and 38.29 (21.95-66.80) for a second dose of mRNA-1273.
For males aged 12 to 39 years, country-specific median time to hospital admission for myocarditis cases was 3 to 7 days (eTable 9 in the Supplement). Comorbid conditions did not differ markedly between vaccinated and unvaccinated myocarditis cases (eTable 10 in the Supplement). Median hospital length of stay was 4 to 5 days for both vaccinated and unvaccinated cases (eTable 11 in the Supplement). For all age groups, the 28-day mortality of the unvaccinated cases with myocarditis was 0.8% (95% CI, 0.3%-2.0%) and ranged from 0.2% (95% CI, 0.0%-0.4%) after the second dose of BNT162b2 to 4.5% (95% CI, 0.0%-13.2%) after the second dose of mRNA-1273; there were no deaths among cases for patients younger than 40 years (eTable 11 in the Supplement).
Discussion
This cohort study of 23.1 million residents across 4 Nordic countries showed higher rates of myocarditis and pericarditis within 28 days after being vaccinated with SARS-CoV-2 mRNA vaccines compared with being unvaccinated. The risks of myocarditis and pericarditis were highest within the first 7 days of being vaccinated, were increased for all combinations of mRNA vaccines, and were more pronounced after the second dose. A second dose of mRNA-1273 had the highest risk of myocarditis and pericarditis, with young males aged 16 to 24 years having the highest risk.
Myocarditis after mRNA vaccination was rare in this study cohort and even among young males. The risk of myocarditis following the mRNA vaccines has been evaluated by the US Food and Drug Administration, which concluded that the benefits of vaccination outweigh the risks and fully authorized the use of mRNA-1273 in persons 18 years or older and BNT162b2 in persons 16 years or older. In addition, BNT162b2 is authorized for emergency use in children 5 years or older.20,21 The European Medicines Agency concluded that the benefits of vaccination outweigh the risks and approved mRNA-1273 for use in persons 12 years or older and BNT162b2 for those 5 years or older.22,23 In addition, a comment published by the American College of Cardiology24 evaluated vaccine-associated myocarditis risk and concluded that the benefits of vaccination outweigh the risks. As of January 2022, there have been nearly 5.8 million deaths associated with COVID-19 worldwide since the start of the pandemic.25 All currently available SARS-CoV-2 mRNA vaccines are highly effective against severe COVID-19 and provide some protection against transmission and infection.26–28 There is some evidence that the mRNA-1273 vaccine, possibly owing to its higher concentration of mRNA, is associated with increased immunogenicity and effectiveness.29,30 This more profound immune response could be one reason for the higher risk of myocarditis, but this hypothesis needs to be investigated further.
Our findings are consistent with higher risk after the second dose and higher risk in young males.2,3,10,11,31–36 Excess events within 28 days in males aged 16 to 24 years of 5.55 events per 100 000 vaccinees after the second dose with BNT162b2 and 18.39 events per 100 000 vaccinees after the second dose with mRNA-1273 are among the highest reported.3,4,32,33 Our finding of a higher risk of myocarditis after mRNA-1273 than after BNT162b2 in this group is in line with data from the US, Canada, France, and England.5,10,11,33,35 In comparison with previous studies, we had the advantage of data analyzed according to a common protocol from 4 different countries, and that showed similar directions of associations, despite considerable differences in prior SARS-CoV-2 infection levels and lockdown policies.
Strengths and Limitations
The main strengths of our study include the population-based cohort design in 4 Nordic countries, large sample size, near-complete follow-up, and independent ascertainment of vaccinations and diagnoses from nationwide registers with mandatory reporting. The findings in the meta-analyses were supported by consistent findings across all 4 countries, despite some country-specific differences in data sources, SARS-CoV-2 transmission, testing activities, and vaccination schedules.
There are also some limitations of the study. We defined events as an inpatient hospital admission with a corresponding main or secondary discharge diagnosis of myocarditis or pericarditis. Diagnostic codes have been shown to have 85% positive predictive value among patients younger than 60 years.37 Thus, without access to data on clinical measures, such as troponin levels, diagnostic imaging results, and endomyocardial biopsy, we studied myocarditis as diagnosed in clinical practice and could therefore not assess how many of these patients fulfilled all criteria for receiving a myocarditis diagnosis.38 However, the median hospital length of stay was 4 to 5 days for both unvaccinated and vaccinated patients, enabling sufficient time for adequate diagnostic procedures and indicative of no difference in disease severity between vaccinated and unvaccinated cases. Deaths were rare, with no deaths of persons younger than 40 years. Our findings in children aged 12 to 15 years were limited to relatively few exposed individuals because vaccination in this age group only recently started in most countries.
Surveillance bias, whereby increased focus and media attention on myocarditis as an adverse event after vaccination39 resulted in more subclinical cases being diagnosed, cannot be ruled out. Hence, all studies including data on vaccination and myocarditis after April 25, 2021, are likely prone to this potential surveillance bias. However, in our study, surveillance bias is unlikely to fully explain the differences between the first and second dose, between the 2 mRNA vaccines, and between age groups. Denmark and Norway had lower background incidence rates of myocarditis than Finland and Sweden.
We studied rates of myocarditis after a positive test result for SARS-CoV-2 infection. However, SARS-CoV-2 infection is associated with acute and postacute events other than myocarditis, including hospitalizations, intensive care unit admissions, and death.40 The present study showed increased risk of myocarditis after a positive test result for SARS-CoV-2 infection, and the risk was highest in the older age groups, whereas the risk of myocarditis after vaccination was highest in the younger age groups. However, the estimated risk of any outcome after SARS-CoV-2 infection will be dependent on the testing strategy. If only severe COVID-19 cases are tested, the association with other events will be strengthened owing to selection bias. Therefore, to reduce selection bias in our analyses of myocarditis after SARS-CoV-2 infection, we included only the period from August 2020 onward, when testing was widely available in the Nordic countries.
The 2 mRNA vaccines were used in the Nordic countries according to availability during 2021, and supply was limited during the first months of 2021. Furthermore, vaccination was first provided for older adults. The availability has thus varied across age, calendar months, and countries. The background incidence rate of myocarditis fluctuates with infectious disease burden, being typically higher during the fall and winter.41 Moreover, differences in lockdown measures affecting the spread of SARS-CoV-2 and other viruses could also affect the background incidence rate in both unvaccinated and vaccinated persons. Most of the younger age groups were vaccinated from July to September 2021, and very few during the spring. However, our supplementary model 3 with adjustment for calendar period resulted in wider CIs but did not substantially change the point estimates.
The observed risks of myocarditis and pericarditis are applicable to the current SARS-CoV-2 pandemic situation in the Nordic countries. In other settings, the background incidence of myocarditis and pericarditis and risks following vaccination may differ. Furthermore, we cannot draw conclusions from the study results to predict myocarditis and pericarditis after a third dose or for children younger than 12 years. We captured all hospitalizations for myocarditis and pericarditis in the Nordic countries during the study period; however, without access to data on clinical measures and diagnostic imaging results, future adjudication must assess how many of these patients fulfill all criteria for a myocarditis diagnosis. Although studies on the long-term prognosis of vaccine-associated cases of myocarditis are lacking and are urgently needed, some evidence suggests that the 28-day risk of death, hospital readmission rates, and development of heart failure appear low, especially in the younger age groups.34
Conclusions
In this cohort study of 23.1 million Nordic residents aged 12 years or older, the risk of myocarditis was higher within 28 days of vaccination with both BNT162b2 and mRNA-1273 compared with being unvaccinated, and higher after the second dose of vaccine than the first dose. The risk was more pronounced after the second dose of mRNA-1273 than after the second dose of BNT162b2, and the risk was highest among males aged 16 to 24 years. Our data are compatible with 4 to 7 excess events within 28 days per 100 000 vaccinees after a second dose of BNT162b2, and 9 to 28 excess events within 28 days per 100 000 vaccinees after a second dose of mRNA-1273. The risk of myocarditis associated with vaccination against SARS-CoV-2 must be balanced against the benefits of these vaccines.
Accepted for Publication: February 23, 2022.
Published Online: April 20, 2022. doi:10.1001/jamacardio.2022.0583
Open Access: This is an open access article distributed under the terms of the CC-BY License. © 2022 Karlstad Ø et al. JAMA Cardiology.
Corresponding Author: Rickard Ljung, MD, PhD, MPH, Division of Use and Information, Swedish Medical Products Agency, PO Box 26, SE-751 03 Uppsala, Sweden (rickard.ljung@lakemedelsverket.se).
Author Contributions: Drs Karlstad and Ljung had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Drs Karlstad, Hovi, and Husby contributed equally to this study and are considered co–first authors; Drs Hviid and Ljung contributed equally and are considered co–senior authors.
Concept and design: Karlstad, Hovi, Husby, Selmer, Nohynek, Sundström, Grünewald, Gulseth, Hviid, Ljung.
Acquisition, analysis, or interpretation of data: Karlstad, Hovi, Husby, Härkänen, Selmer, Pihlström, Hansen, Gunnes, Sundström, Wohlfahrt, Nieminen, Grünewald, Gulseth, Hviid, Ljung.
Drafting of the manuscript: Karlstad, Husby, Härkänen, Nohynek, Ljung.
Critical revision of the manuscript for important intellectual content: Karlstad, Hovi, Husby, Härkänen, Selmer, Pihlström, Hansen, Nohynek, Gunnes, Sundström, Wohlfahrt, Nieminen, Grünewald, Gulseth, Hviid.
Statistical analysis: Karlstad, Härkänen, Selmer, Pihlström, Hansen, Gunnes, Sundström, Grünewald, Ljung.
Obtained funding: Gulseth, Hviid.
Administrative, technical, or material support: Karlstad, Nohynek, Gulseth.
Supervision: Hovi, Husby, Nohynek, Wohlfahrt, Hviid, Ljung.
Conflict of Interest Disclosures: Dr Karlstad reported participating in research projects funded by Novo Nordisk and LEO Pharma, all regulator-mandated phase 4 studies with funds paid to his institution and outside the submitted work. Dr Hovi reported being affiliated with the Finnish Institute for Health and Welfare and was thus obligated by legislation to investigate the potential postmarketing harmful effects of vaccines during the conduct of the study. Dr Husby reported receiving funding from the Lundbeck Foundation. Dr Nohynek reported receiving nonfinancial support from WHO SAGE (Strategic Advisory Group of Experts) and the Global Advisory Committee on Vaccine Safety during the conduct of the study; and being employed by the Finnish Institute for Health and Welfare (THL), which receives research funding from Sanofi Pasteur, GlaxoSmithKline, and Pfizer for research studies not related to the current study nor to COVID-19. Dr Sundström reported participating in research funded by governmental agencies, universities, Astellas Pharma, Janssen Biotech, AstraZeneca, Pfizer, Roche, (then) Abbott Laboratories, (then) Schering-Plough, UCB Nordic, and Sobi, with all funds paid to Karolinska Institutet, outside the submitted work. Dr Nieminen reported receiving grants from Sanofi Pasteur outside the submitted work; and being employed by THL. Dr Grünewald reported being involved in the European Medicines Agency regulatory assessment of Comirnaty; being previously employed at a drug development consultancy firm with cross-product responsibilities; and being involved on a project for pertussis vaccines funded by Sanofi Pasteur, Merck Sharp & Dohme Corp, and GlaxoSmithKline at the Swedish Agency of Infectious Disease Control. Dr Gulseth reported participating in research projects and clinical trials funded by Novo Nordisk, GlaxoSmithKline, AstraZeneca, and Boehringer-Ingelheim paid to Oslo University Hospital; and receiving personal fees from Sanofi-Aventis. Dr Hviid reported receiving grants from The Lundbeck Foundation during the conduct of the study. Dr Ljung reported receiving grants from Sanofi Aventis paid to his institution outside the submitted work; and receiving personal fees from Pfizer outside the submitted work. No other disclosures were reported.
Additional Information: Among us, Dr Hviid had full access to all the Danish data, Dr Hovi had full access to all the Finnish data, Dr Karlstad had full access to all the Norwegian data, Dr Ljung had full access to all the Swedish data, and Dr Härkänen had full access to all the meta-analyses data in the study, and each investigator takes responsibility for the integrity of the data and the accuracy of the respective analyses. In addition, Drs Husby, Hansen, and Wohlfahrt, of the Statens Serum Institut, analyzed the Danish data and are responsible for those analyses; Drs Karlstad, Selmer, and Gunnes, of the Norwegian Institute of Public Health, conducted and are responsible for the analyses of the Norwegian data; Drs Hovi and Härkänen, of the Finnish Institute for Health and Welfare, conducted and are responsible for the analyses of the Finnish data; and Drs Pihlström, Sundström, Grünewald, and Ljung, of the Swedish Medical Products Agency, conducted and are responsible for the analyses of the Swedish data.

References
ArticlePubMedGoogle ScholarCrossref
ArticlePubMedGoogle ScholarCrossref
ArticlePubMedGoogle ScholarCrossref
Um höfund

- Sigurlaug Ragnarsdóttir
- ✞༺(((( Ⓒilla ℜągnąℜṧ )))༻♚༺ BA Classical Art Historian || MA Culture & Media || Tourism & Sales Management || Web Design || Photo & Videographer for Tourism Magasins ༻
Síðustu færslur
 PROTECT THE CHILDREN23. nóvember, 2024BARNAMÁLARÁÐSTEFNAN 2024
PROTECT THE CHILDREN23. nóvember, 2024BARNAMÁLARÁÐSTEFNAN 2024 MANNRÉTTINDI19. nóvember, 2024MENNTASPJALL VALGERÐAR SNÆLAND JÓNSDÓTTUR
MANNRÉTTINDI19. nóvember, 2024MENNTASPJALL VALGERÐAR SNÆLAND JÓNSDÓTTUR MANNRÉTTINDI9. ágúst, 2024Lög um borgaralega handtöku voru felld úr gildi árið 2008
MANNRÉTTINDI9. ágúst, 2024Lög um borgaralega handtöku voru felld úr gildi árið 2008 Sameinuðu Þjóðirnar28. desember, 2023Lestrarefni Menntamálastofnunar: Varúð hér býr vampíra – auðlesin sögubók á léttu máli og bókinni fylgir verkefnahefti sem hægt er að vinna samhliða lestri.
Sameinuðu Þjóðirnar28. desember, 2023Lestrarefni Menntamálastofnunar: Varúð hér býr vampíra – auðlesin sögubók á léttu máli og bókinni fylgir verkefnahefti sem hægt er að vinna samhliða lestri.